Detection
Diagnosing Uterine Fibroids
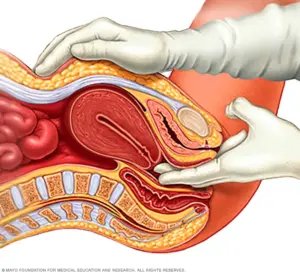
Uterine fibroids are frequently found during a routine pelvic exam. Your doctor may feel irregularities in the shape of your uterus, suggesting the presence of fibroids. You may suspect the presence of uterine fibroids based on symptoms that you are experiencing.
You are not alone.
By age 50, nearly two-thirds of women experience uterine fibroids
Fibroids can be diagnosed using various tests such as²:
-
Ultrasound
It uses soundwaves to create a picture of the uterus and other pelvic organs. A doctor or technician moves the ultrasound device over your abdomen (transabdominal) or places it inside your vagina (transvaginal) to get images of your pelvic organs including your uterus. An ultrasound is the most frequent test utilized to diagnose fibroids, however, it does not always provide a comprehensive picture the pictures or information needed of your uterus. More detailed tests are MRI and hysteroscopy.
-
Magnetic resonance imaging (MRI)
This imaging test can show in more detail the size and location of fibroids, identify different types of tumors and help determine appropriate treatment options. We recommend MRI is recommended since it shows the fibroid as well as the blood supply to the fibroid. This more comprehensive imaging is important for surgical planning.
-
Hysteroscopy
Uses a slender device (the hysteroscope) to see the inside of the uterus. It is inserted through the vagina and cervix (opening of the uterus). This allows your healthcare professional to see fibroids inside the uterine cavity.
-
Lab Tests
If you have abnormal menstrual bleeding, your doctor may order other tests to investigate potential causes. These might include a complete blood count (CBC) to determine if you have anemia because of chronic blood loss and other blood tests to rule out bleeding disorders or thyroid problems.
Less frequently used imaging methods are:
Hysterosalpingography:
This is a special X-ray test. It may detect abnormal changes in the size andshape of the uterus and fallopian tubes.
Sonohysterography:
A test in which fluid is put into the uterus through the cervix. Ultrasonography is then used to show the inside of the uterus. The fluid provides a clear picture of the uterine lining.
Laparoscopy:
Uses a slender device (the laparoscope) to help your health care professional see the inside of the abdomen. It is inserted through a small cut just below or through the navel.Fibroids on the outside of the uterus can be seen with the laparoscope.Imaging tests, such as magnetic resonance imaging and computed tomography scans, may be used but are rarely needed. Some of these tests may be used to track the growth of fibroids over time.
Menorrhagia + Anemia
Why am I passing clots?

Unfortunately, clots with fibroids is very common because fibroids can cause changes in the way that your blood vessels and clotting mechanisms work during your period. The causes of HMB in UF are not well known, abnormal development of the inner layer of your uterus called endometrium and altered clotting mechanisms may be a factor.
Learn more. Are there risk factors?
Some women have specific genes that may predispose them, and their families, to fibroids; and lifestyle and reproductive factors influence fibroids. Some fibroids grow with time and others shrink. Fibroids can also have growth spurts where they grow quickly over a short period of time.
What happens next?
Don’t wait to seek treatment because symptoms could get worse.
What questions should I ask my doctor?
- How many fibroids do I have?
- What size is my fibroid(s)?
- Where is my fibroid(s) located (outer surface, inner surface, or in the wall of the uterus)?
- Can I expect the fibroid(s) to grow larger?
- How rapidly have they grown (if they were known about already)?
- How will I know if the fibroid(s) is growing larger?
- What problems can the fibroid(s) cause?
- What tests or imaging studies are best for keeping track of the growth of my fibroids?
- What are my treatment options if my fibroid(s) becomes a problem?
- What fibroid surgery options do you specialize in?
- May I speak with a patient who has had the same surgery that you are recommending for me?
- What happens to fibroids when you get to menopause?
- A second opinion is always a good idea if your doctor has not answered your questions completely or does not seem to be meeting your needs.
What should my doctor ask me?
- How are you feeling?
- What symptoms are most troublesome?
- Can you rank your goals for treatment? Ex: eliminate pain, stop heavy menstrual bleeding, relief from pain during intercourse, desire to conceive.
You are not alone
By age 50, nearly two-thirds of women experience uterine fibroids¹
Join Our Community